Can Physiotherapy Help Spinal Stenosis? An Evidence Based Approach
- Nirvan Maharjan

- Apr 18
- 2 min read
Lumbar spinal stenosis is a common condition, especially in older adults, often presenting as back pain with leg symptoms such as heaviness, numbness, or pain while walking. Many people are told that surgery is inevitable—but the evidence suggests otherwise.

What Is Spinal Stenosis?
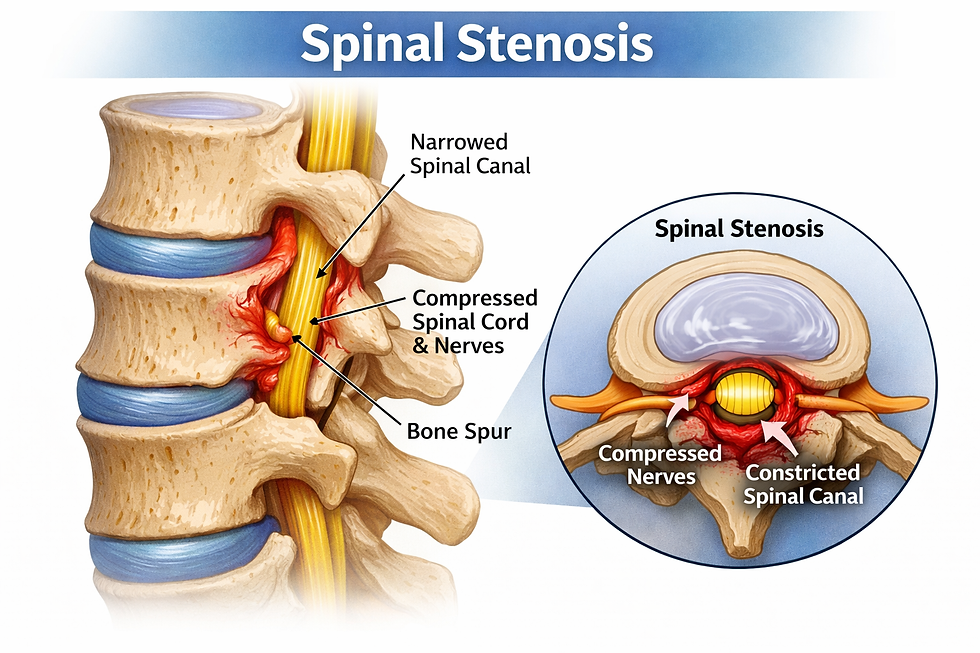
Spinal stenosis refers to a narrowing of the spinal canal that can compress nerves. In clinical practice, it is often grouped under a broader classification system rather than treated purely as a structural diagnosis.
Within Mechanical Diagnosis and Therapy (MDT), spinal stenosis is considered part of the “OTHER” subgroup, meaning management depends more on how symptoms respond to movement rather than imaging findings alone.
Why Diagnosis Alone Isn’t Enough
Research shows that relying only on scans (like MRI) can be misleading. Many people have structural changes without symptoms, and high use of imaging is not recommended as first-line care.
Instead, what matters more is:
How your pain behaves
What movements make it better or worse
Your functional limitations (like walking or standing)
What Does the Evidence Recommend?
Modern guidelines strongly support conservative management as the first step for most spinal conditions, including stenosis.
Recommended first-line strategies include:
Exercise therapy
Education and reassurance
Staying active
Self-management strategies
Addressing psychosocial factors
These approaches are consistently supported in the literature.
On the other hand, early reliance on:
Imaging
Rest
Injections
Surgery
is generally not recommended unless absolutely necessary.
How Physiotherapy Helps
Physiotherapy—especially when guided by MDT principles—focuses on identifying how your body responds to movement.
For example:
Some patients improve with flexion-based movements (bending forward)
Others may respond differently depending on their classification
This concept, known as directional preference, is key to guiding treatment and improving outcomes.
The Role of Movement and Function
Spinal stenosis often presents with:
Pain during walking or standing
Relief when sitting or bending forward
These patterns are important because they guide targeted treatment rather than a one-size-fits-all approach.
Research also highlights that functional limitations and leg pain are important prognostic factors—meaning they influence recovery outcomes.
Can You Avoid Surgery?
Many patients improve significantly with conservative care. Studies in MDT-based care show:
Reduced need for imaging.
Lower rates of injections and surgery
Better long-term outcomes when patients are actively involved in their recovery
Surgery may still be necessary in some cases—but it is not the first or only option.
Key Takeaway
Spinal stenosis is not just a structural problem—it’s a condition that should be managed based on how your body responds to movement and activity.
The best outcomes come from:
Staying active
Following a personalized exercise plan
Understanding your condition
Working with a physiotherapist who uses evidence-based assessment
If you’re experiencing back or leg pain and have been told you have spinal stenosis, a proper mechanical assessment can help determine the best path forward—often without the need for invasive treatments.




Comments